Mastectomy – What You Need to Know
If you’re facing a mastectomy or considering a mastectomy, we have information to help. Here, we cover the types of mastectomy, the surgical procedure, what to expect after surgery, support, resources and more.
Frequently Asked Questions on Mastectomy |
|
What is a mastectomy? A mastectomy is surgery to remove one or both breasts. The surgeon removes all the breast tissue. In most cases, the nipple and areola are also removed. Learn more about the surgical procedure). Why might I have a mastectomy? A mastectomy can be used to treat breast cancer. It can be used to treat ductal carcinoma in situ (DCIS), invasive breast cancer or breast cancer that has returned. It can also be used to lower the risk of breast cancer in women who haven’t been diagnosed with breast cancer but are at high risk. What should I expect after surgery? You will have some pain and numbness, and you may have limited range of motion in the shoulder area. Learn more about what to expect after a mastectomy both physically and emotionally. |
Learn more about:
- Mastectomy for breast cancer treatment
- Mastectomy for breast cancer risk reduction
- Types of mastectomy
- Mastectomy surgery
- Breast reconstruction
- Breast prosthesis
- Going flat
- Length of hospital stay
- What to expect after a mastectomy
- Questions to ask your health care provider before and after surgery
- Support and resources
Mastectomy for breast cancer treatment
A mastectomy is an option for people who have:
- Ductal carcinoma in situ (DCIS)
- Invasive breast cancer (non-metastatic)
- Inflammatory breast cancer
- Paget disease of the breast (Paget disease of the nipple)
A mastectomy is also used to treat breast cancer that has recurred (come back) after treatment with a lumpectomy plus radiation therapy.
Learn about the types of mastectomy.
Learn about mastectomy surgery.
Read our fact sheet on breast cancer surgery.
Radiation therapy
Some women who have a mastectomy will not need radiation therapy.
However, in some cases, radiation therapy is used after a mastectomy to treat the chest wall, the axillary lymph nodes (the lymph nodes in the underarm area) and/or the lymph nodes around the collarbone.
If your treatment plan includes chemotherapy, you’ll have radiation therapy after you finish chemotherapy.
When is a lumpectomy plus radiation therapy an option to a mastectomy?
Some women have the option of a mastectomy or a lumpectomy (also called breast-conserving surgery), and choose a mastectomy. For other women, a mastectomy is the only breast cancer surgery option.
Some women can have a lumpectomy plus radiation therapy instead of a mastectomy.
Learn about deciding between a lumpectomy and a mastectomy.
Risk-reducing mastectomy
Risk-reducing contralateral mastectomy
A risk-reducing (prophylactic) contralateral mastectomy is the removal of the contralateral (opposite) breast in a person who has breast cancer in only one breast. It’s usually done at the same time as breast cancer surgery, so both breasts are removed during the same surgery.
The goal of a risk-reducing contralateral mastectomy is to try and prevent breast cancer in the contralateral breast of a woman who has a very high risk of breast cancer. However, removing the contralateral breast does not lower the risk of dying from the original breast cancer [7]. Removing the contralateral breast also does not lower the risk of the original breast cancer spreading beyond the breast and nearby lymph nodes to other parts of the body (most often the bones, lungs, liver or brain). This is called metastatic breast cancer.
The National Comprehensive Cancer Network (NCCN) recommends a risk-reducing contralateral mastectomy only be considered for women who have a very high risk of breast cancer due to an inherited gene mutation in one of these genes [8]:
- BRCA1
- BRCA2
- CDH1
- PALB2
- PTEN
- STK11
- TP53
Cosmetic reasons for surgery to the contralateral breast
Sometimes, there may be cosmetic reasons to consider surgery to the contralateral breast. For example, some women may choose breast reduction to the contralateral breast to create a more even look with a reconstructed breast.
Learn more about breast reconstruction.
Risk-reducing bilateral mastectomy
Women with a BRCA1, BRCA2 or certain other inherited gene mutations who haven’t been diagnosed with breast cancer, may have both breasts removed to prevent breast cancer. This is called a risk-reducing bilateral mastectomy.
Learn more about a risk-reducing bilateral mastectomy.
Types of mastectomy
There are 2 main types of mastectomy: total (simple) and modified radical. Your diagnosis guides the type of mastectomy you will have.
The figure below shows the types of mastectomy and describes when each is used.
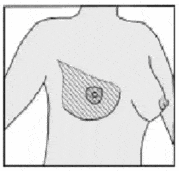 |
Total (simple) mastectomy The surgeon removes the entire breast and the lining of the chest muscle, but no other tissue. For some women, much of the skin of the breast may be left intact for breast reconstruction. This is called a skin-sparing mastectomy. In some cases, the nipple may also be left intact. This is called a nipple-sparing mastectomy. A sentinel lymph node biopsy may be done, or no lymph nodes may be removed, depending on the breast cancer. A total (simple) mastectomy may be used to treat:
A total mastectomy is also used for women at high risk who have a risk-reducing mastectomy. Sometimes breast reconstruction is done at the same time as a mastectomy. |
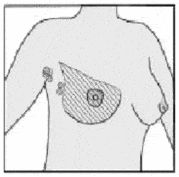 |
Modified radical mastectomy The surgeon removes the entire breast, the lining of the chest muscles and the axillary lymph nodes (the lymph nodes in the underarm area). A modified radical mastectomy may be used to treat:
Sometimes, breast reconstruction is done at the same time as a mastectomy. With inflammatory breast cancer, breast reconstruction can’t be done at the same time as a mastectomy. However, it may be done at a later time. |
Skin-sparing mastectomy and nipple-sparing mastectomy
If you’re having breast reconstruction at the same time as a mastectomy, the surgeon may be able to use a skin-sparing technique, or possibly a nipple-sparing technique.
A skin-sparing mastectomy removes all the breast tissue but saves much of the skin of the breast. The plastic surgeon can use this skin as an envelope to help form the reconstructed breast.
A nipple-sparing mastectomy is a skin-sparing mastectomy that also preserves the nipple and areola.
Mastectomy – the procedure
A mastectomy is the surgical removal of the entire breast.
With a mastectomy, the surgeon removes all the breast tissue. In most, but not all cases, the nipple and areola are also removed.
Mastectomy surgery
A mastectomy is performed under general anesthesia. This means you’re asleep during the surgery.
The surgeon removes all the breast tissue. In most, but not all cases, the nipple and areola are also removed.
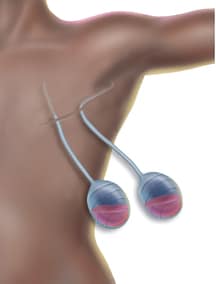
The surgeon closes the skin with stitches and puts in 1-2 surgical drains (tubes) so fluid from the wound can drain out (see image below). The drain(s) stays in for about a week to 10 days after surgery.
|
Image courtesy of Lange Productions (http://langeproductions.com/). |
Assessing tumor margins
A pathologist checks the tissue removed during breast surgery. It takes about 1-2 weeks to do a complete check of the tissue.
By looking at the tissue under a microscope, the pathologist determines whether there are cancer cells in the margins (the rim of tissue around the tumor).
Whether or not the margins contain cancer cells doesn’t usually affect treatment after a mastectomy since the entire breast is removed.
However, in rare cases after a mastectomy, the deep margin (the margin closest to the chest wall) or the superficial margin (the skin margin) contains cancer cells. In these cases, more surgery and/or radiation therapy may be recommended.
With a nipple-sparing mastectomy, whether or not the nipple margin (the margin closest to the nipple) contains cancer cells can affect treatment. If the nipple margin contains cancer cells, more surgery is recommended.
Learn more about assessing tumor margins.
Assessing lymph nodes (Has the cancer spread to the lymph nodes?)
If breast cancer spreads, the axillary lymph nodes (the lymph nodes in the underarm area) are the first place it’s likely to go.
During a mastectomy for invasive breast cancer, some of the axillary lymph nodes are removed to check for cancer cells. The presence or absence of cancer in these nodes is an important factor in cancer staging and the chances for survival.
Learn more about assessing axillary lymph nodes.
Read our fact sheet on axillary lymph nodes.
Ductal carcinoma in situ (DCIS) and sentinel lymph node biopsy
A sentinel lymph node biopsy removes some axillary lymph nodes so they can be checked for cancer cells. When a mastectomy is used to treat DCIS (a non-invasive breast cancer), a sentinel lymph node biopsy is be done. This helps some people avoid an axillary lymph node dissection (a more invasive surgery to remove axillary lymph nodes) later.
Once a mastectomy has been done, a person can’t have a sentinel lymph node biopsy.
If it turns out there’s invasive breast cancer (along with DCIS) in the tissue removed during the mastectomy, and a sentinel lymph node biopsy wasn’t done, an axillary lymph node dissection might be needed. So, having a sentinel lymph node biopsy helps some people avoid an axillary lymph node dissection.
Learn more about sentinel lymph node biopsy during a mastectomy for DCIS.
Mastectomy with breast reconstruction
Some women choose to have breast reconstruction to help restore the look of the breast that was removed.
Reconstruction may be immediate (done at the same time as the mastectomy) or delayed (done at a later time). In general, cosmetic results are better with immediate reconstruction [318].
If you want reconstruction, find out if there’s a plastic surgeon available who specializes in breast reconstruction. This may be important when making a decision about surgery. Discuss your reconstruction options with your plastic surgeon before your breast surgery.
Not all women choose to have reconstructive surgery. Some women choose to get a breast prosthesis. Others choose to have a flat closure (“go flat”).
Learn more about breast reconstruction.
Learn about insurance coverage and financial assistance for breast reconstruction.
Read our fact sheet on breast reconstruction or prosthesis after a mastectomy.
Mastectomy with breast prosthesis
Read our blog, Christy’s Story: Why I Chose Not to Have Breast Reconstruction.
If you don’t have breast reconstruction, you can get a breast prosthesis that best fits your lifestyle. This is a breast form made of silicone gel, foam or other materials that’s fitted to your chest.
A prosthesis is usually worn in the pocket of a special bra, but it may also placed directly on top of your skin with a stick-on patch.
The surgeon will leave the area as flat as possible so the prosthesis can be comfortably fitted to your chest.
Your prosthesis can be properly fitted several weeks after your mastectomy surgery.
Your health care provider can discuss your breast prosthesis options with you.
Visit the FORCE website for a photo gallery of images of people after a mastectomy.
Learn about insurance coverage for breast prosthesis and financial assistance for breast prosthesis.
Read our fact sheet on breast reconstruction or prosthesis after a mastectomy.
Breast prosthesis and air travel |
Susan G. Komen® wants to make sure people who have breast cancer are treated with respect and dignity. When you travel by air, these steps may be helpful:
Learn about TSA screening if you wear a wig, scarf or other head covering. Learn about TSA screening if you wear a compression sleeve. If you have concerns about airline security screening, visit the TSA website. |
Mastectomy with a flat closure
If you don’t want to have breast reconstruction or use a breast prosthesis after a mastectomy, you can have a flat closure. This is also called going flat.
With a flat closure, the skin remaining after a mastectomy is tightened and smoothed to flatten out the chest wall as much as possible. However, the area will not be completely flat or smooth. How flat the area will be after surgery varies from person to person. There will also be a scar.
Talk with your health care provider about your surgery options. If you choose to go flat, talk with your surgeon before breast surgery.
Read our blog, Despite What Doctors Told Me, I’ve Never Regretted My Decision to Go Flat After a Double Mastectomy.
Read our blog, Going Flat? Self-Advocacy is Key.
Length of hospital stay
Most people stay in the hospital overnight after a mastectomy.
If breast reconstruction is done, the stay may be longer, depending on the type of reconstruction you have.
Discuss the expected length of stay with your surgeon, plastic surgeon (if you’re having reconstruction) and insurance company.
Learn more about insurance issues related to a mastectomy and breast reconstruction.
What to expect after a mastectomy
Pain and numbness
After a mastectomy (with or without breast reconstruction), you’ll have some soreness in your chest, underarm and shoulder.
You will be numb across your chest (from your collarbone to the top of your rib cage). Unfortunately, this numbness usually doesn’t go away. You may get some feeling back over time, but it will never be the same as before surgery.
If axillary lymph nodes (lymph nodes in the underarm area) are removed during surgery, you may also have some numbness and a burning feeling under and behind your arm.
Pain related to surgery may be treated with mild pain relievers or if the pain is more severe, prescription medication.
If axillary lymph nodes were removed during surgery, you may also have some numbness and a burning feeling under and behind your arm.
Learn more about the management of surgery-related pain.
Range of motion in the shoulder area
If you had a sentinel lymph node biopsy to remove axillary lymph nodes during surgery, you may have some short-term problems with your range of motion in your shoulder area (the ability to move the shoulder easily).
If you had an axillary lymph node dissection, your health care provider may recommend special exercises to improve your range of motion. They may also refer you to a physical therapist if needed.
With an axillary lymph node dissection, problems with range of motion in the shoulder area may last longer than with a sentinel lymph node biopsy.
Risk of lymphedema
If axillary lymph nodes are removed during surgery, there’s a risk of lymphedema.
Lymphedema is a condition where fluid builds up in the arm and/or hand, causing it to swell. Today, lymphedema isn’t very common. If it does occur, it usually develops within 3 years of having axillary lymph nodes removed [5-6].
Learn more about lymphedema.
Emotional health after a mastectomy
After a mastectomy, you may feel a buildup of emotions. You may have been anxious leading up to surgery. And, after surgery, you may feel a sense of relief or you may be worried about what happens next. This is normal.
Make sure you take time to recover both emotionally and physically. You may want to have family and friends available for support.
Learn more about social support.
Treatment guidelines
Although the exact treatment for breast cancer varies from person to person, evidence-based guidelines help make sure high-quality care is given. These guidelines are based on the latest research and agreement among experts.
The National Comprehensive Cancer Network (NCCN) and the American Society of Clinical Oncology (ASCO) are respected organizations that regularly review and update their guidelines.
In addition, the National Cancer Institute (NCI) has treatment overviews.
Talk with your health care team about which treatment guidelines they follow.
After you get a recommended treatment plan from your health care team, study your treatment options. Together with your health care team, make thoughtful, informed decisions that are best for you. Each treatment has risks and benefits to consider along with your own values and lifestyle.
You’re not alone
If you’re facing breast cancer surgery, it’s normal to feel worried or afraid. Many people have been where you are today. They had the same fears and faced the same tough choices. They’ve gone through breast cancer treatment and are living their lives.
It may help to talk with others who’ve finished treatment to help ease your fears. You can do this in a support group or by connecting one-on-one with another breast cancer survivor.
You can also talk with your health care providers about how you’re coping. They care about your overall well-being and can help you find ways to improve it. In addition to suggesting a support group, they may connect you to another member of your health care team, such as a social worker or patient navigator, for support. They may also refer you to a counselor.
Our Support section has a list of resources to help you find local and online support groups and other resources.
Learn more about social support and support groups.
Learn about ways to cope with stress.
Resources
Transportation, lodging, childcare and eldercare assistance
You may not live near the hospital where you’ll have your surgery. It’s OK to ask for help.
There may be resources available if you need a ride to and from surgery or help with childcare or eldercare. Family and friends often want to help but don’t know how. These are great ways for them to get involved.
There may be some programs that help with local or long-distance transportation and lodging (if you need a place to stay overnight).
There may also be programs to help you with childcare or eldercare costs.
Learn more about transportation, lodging, childcare and eldercare assistance programs.
Educational resources
Find:
- A list of questions you may want to ask your health care provider before and after surgery
- Our Questions to Ask Your Doctor About Breast Surgery resource
- Our Questions to Ask Your Doctor About Breast Reconstruction resource
Read our fact sheets on:
- Breast cancer surgery
- Breast reconstruction or prosthesis after a mastectomy
- Axillary lymph nodes
- Support after a breast cancer diagnosis
Watch our BC101 interactive video on mastectomy.
Susan G. Komen® Support Resources |
|
Updated 04/13/24